Items filtered by date: November 2021
The Three Grades of Ankle Sprains
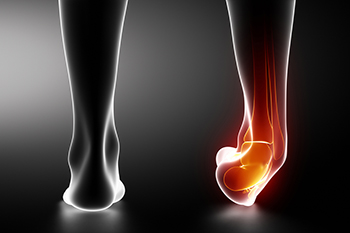 When the ligaments that connect the bones to each other become overstretched or torn, a sprain can occur. When it comes to ankle sprains, they can be diagnosed as one of 3 different categories. When the ligament is only mildly stretched, this is known as a Grade 1 sprain. Once the ligament is even slightly torn, it is considered a Grade 2 sprain. A Grade 3 ankle sprain can occur when the ligament is completely torn. Common signs of a sprained ankle may include pain, tenderness, bruising, stiffness, and an inability to bear weight. Because the symptoms of a sprain are often similar to that of a fracture, patients who believe that they have sprained their ankle should consult with a podiatrist in order to make sure they do not have any broken bones. A podiatrist will be able to assess the severity of the injury and provide a proper treatment option.
When the ligaments that connect the bones to each other become overstretched or torn, a sprain can occur. When it comes to ankle sprains, they can be diagnosed as one of 3 different categories. When the ligament is only mildly stretched, this is known as a Grade 1 sprain. Once the ligament is even slightly torn, it is considered a Grade 2 sprain. A Grade 3 ankle sprain can occur when the ligament is completely torn. Common signs of a sprained ankle may include pain, tenderness, bruising, stiffness, and an inability to bear weight. Because the symptoms of a sprain are often similar to that of a fracture, patients who believe that they have sprained their ankle should consult with a podiatrist in order to make sure they do not have any broken bones. A podiatrist will be able to assess the severity of the injury and provide a proper treatment option.
Although ankle sprains are common, they aren’t always minor injuries. If you need your ankle injury looked at, contact Dr. Douglas Mckay from New Jersey . Our doctor can provide the care you need to keep you pain-free and on your feet.
How Does an Ankle Sprain Occur?
Ankle sprains are the result of a tear in the ligaments within the ankle. These injuries may happen when you make a rapid shifting movement while your foot is planted. A less common way to sprain your ankle is when your ankle rolls inward while your foot turns outward.
What Are the Symptoms?
- Pain at the sight of the tear
- Bruising/Swelling
- Ankle area is tender to touch
- In severe cases, may hear/feel something tear
- Skin discoloration
Preventing a Sprain
- Wearing appropriate shoes for the occasion
- Stretching before exercises and sports
- Knowing your limits
Treatment of a Sprain
In many cases, the RICE method (Rest, Ice, Compression, and Elevate) is used to treat ankle sprains. However, you should see a podiatrist to see which treatment option would work best with your injury. In severe cases, surgery may be required.
It is important to ask your doctor about rehab options after you receive treatment for your injury. Stretching, strength training, and balance exercises may help the ankle heal while also preventing further injury.
If you have any questions, please feel free to contact one of our offices located in Caldwell, and Galloway, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Keeping Your Heels Soft to Prevent Them From Cracking
When you apply weight to your foot, the skin on your heels expands. If this skin is dry and lacking elasticity, cracks in the skin may eventually form. Dry, cold weather, obesity, open-back shoes, standing on hard floors for an extended period of time, and conditions that cause dry skin can all contribute to heels becoming stiff and cracked. To avoid getting cracked heels, keep them moisturized. The best way to seal in moisture is to apply ointment or cream—containing hyaluronic or lactic acid, mineral oil, lanolin or petrolatum—right after a shower or bath. If your heels are already thickened and cracked, you can try to thin them down by gently rubbing them with a pumice stone or applying a keratolytic agent, unless you have diabetes, nerve damage, or poor circulation. If cracked heels are allowed to deepen, they may become painful and bleed, and possibly even become infected. If your cracked heels have progressed to this point, or you need help getting them smooth and supple again, make an appointment with your local podiatrist.
Cracked heels are unsightly and can cause further damage to your shoes and feet. If you have any concerns, contact Dr. Douglas Mckay from New Jersey . Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
Cracked heels appear unappealing and can make it harder for you walk around in sandals. Aside from looking unpleasant, cracked heels can also tear stockings, socks, and wear out your shoes. There are several methods to help restore a cracked heel and prevent further damage.
How Do You Get Them?
Dry skin is the number one culprit in creating cracked heels. Many athletes, walkers, joggers, and even swimmers suffer from cracked heels. Age and skin oil production play a role to getting cracked heels as well.
Promote Healing
Over the counter medicines can help, especially for those that need instant relief or who suffer from chronic dry feet.
Wear Socks – Wearing socks with medicated creams helps lock in moisture.
Moisturizers – Applying both day and night will help alleviate dryness which causes cracking.
Pumice Stones – These exfoliate and remove dead skin, which allows for smoother moisturizer application and better absorption into the skin.
Change in Diet
Eating healthy with a well-balanced diet will give the skin a fresh and radiant look. Your body responds to the kinds of food you ingest. Omega-3 fatty acids and zinc supplements can also revitalize skin tissue.
Most importantly, seek professional help if unsure how to proceed in treating cracked heels. A podiatrist will help you with any questions or information needed.
If you have any questions, please feel free to contact one of our offices located in Caldwell, and Galloway, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
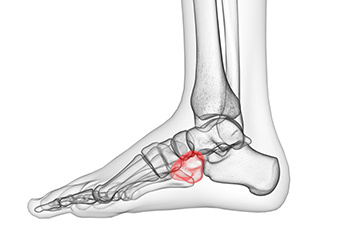
What Is Cuboid Syndrome?
The cuboid bone is a tiny, cube-shaped (cuboidal) bone, which is one of the seven tarsal bones of the foot. It is located on the outside of the foot, roughly halfway between the pinky toe and the heel. The cuboid bone moves slightly during normal foot motion, however, forceful movements or certain positions that are maintained for prolonged periods of time can cause the cuboid bone to shift excessively and therefore it becomes dislocated. This is known as cuboid syndrome. Symptoms may include pain and possibly swelling on the lateral (outside) part of the foot which increases when walking or standing. It may even be difficult or impossible to walk. Podiatrists may use a “whip” procedure to quickly and firmly apply force to the cuboid bone to get it back into alignment as the patient relaxes in a prone position. If you believe you may be suffering from cuboid syndrome, contact a podiatrist.
Cuboid syndrome, also known as cuboid subluxation, occurs when the joints and ligaments near the cuboid bone in the foot become torn. If you have cuboid syndrome, consult with Dr. Douglas Mckay from New Jersey . Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Cuboid syndrome is a common cause of lateral foot pain, which is pain on the outside of the foot. The condition may happen suddenly due to an ankle sprain, or it may develop slowly overtime from repetitive tension through the bone and surrounding structures.
Causes
The most common causes of cuboid syndrome include:
- Injury – The most common cause of this ailment is an ankle sprain.
- Repetitive Strain – Tension placed through the peroneus longus muscle from repetitive activities such as jumping and running may cause excessive traction on the bone causing it to sublux.
- Altered Foot Biomechanics – Most people suffering from cuboid subluxation have flat feet.
Symptoms
A common symptom of cuboid syndrome is pain along the outside of the foot which can be felt in the ankle and toes. This pain may create walking difficulties and may cause those with the condition to walk with a limp.
Diagnosis
Diagnosis of cuboid syndrome is often difficult, and it is often misdiagnosed. X-rays, MRIs and CT scans often fail to properly show the cuboid subluxation. Although there isn’t a specific test used to diagnose cuboid syndrome, your podiatrist will usually check if pain is felt while pressing firmly on the cuboid bone of your foot.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are ice therapy, rest, exercise, taping, and orthotics.
If you have any questions, please feel free to contact one of our offices located in Caldwell, and Galloway, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
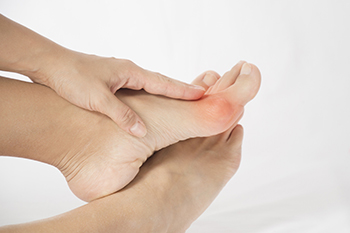
What to Consider Before Bunion Surgery
A bunion is a common foot deformity characterized by a bony bump that forms at the base of the big toe joint. The bump can become inflamed, red, swollen, and painful. It also pushes the big toe out of alignment, so that it is tilted toward the smaller toes instead of pointing straight ahead. Bunions progressively worsen without treatment, and surgery is often the only option to permanently remove them. That said, there are many things to consider prior to making the decision to operate. Certain underlying health conditions, such as diabetes, rheumatoid arthritis, and gout, can increase the risk of complications from surgery. It is also important to think about your lifestyle. Do you intend to wear high heels, exercise, or stand for prolonged periods of time? These factors can help your podiatrist determine if bunion surgery is the right treatment option for you. For more information about bunions, please consult with a podiatrist.
If you are suffering from bunion pain, contact Dr. Douglas Mckay of New Jersey . Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
- Genetics – some people inherit feet that are more prone to bunion development
- Inflammatory Conditions - rheumatoid arthritis and polio may cause bunion development
Symptoms
- Redness and inflammation
- Pain and tenderness
- Callus or corns on the bump
- Restricted motion in the big toe
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact one of our offices located in Caldwell, and Galloway, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
The Spreading of Athlete’s Foot
 Athlete’s foot is a very contagious fungal infection that often thrives in warm moist environments such as showers, locker rooms, and swimming pools, and it can spread from things such as towels, floors, and clothing. Unless the feet have been washed and dried thoroughly, fungal spores can penetrate any fissures or sores and begin to spread. The infection may also spread by hand to other parts of the body when it is scratched or touched. Because of how easily it spreads, good foot hygiene is one of the most important factors to prevent Athlete’s foot. As a result of Athlete’s foot, the feet can become dry and flaky, and they will get itchy and scaly. Patients who have Athlete’s foot should visit a podiatrist to properly treat the infection.
Athlete’s foot is a very contagious fungal infection that often thrives in warm moist environments such as showers, locker rooms, and swimming pools, and it can spread from things such as towels, floors, and clothing. Unless the feet have been washed and dried thoroughly, fungal spores can penetrate any fissures or sores and begin to spread. The infection may also spread by hand to other parts of the body when it is scratched or touched. Because of how easily it spreads, good foot hygiene is one of the most important factors to prevent Athlete’s foot. As a result of Athlete’s foot, the feet can become dry and flaky, and they will get itchy and scaly. Patients who have Athlete’s foot should visit a podiatrist to properly treat the infection.
Athlete’s Foot
Athlete’s foot is often an uncomfortable condition to experience. Thankfully, podiatrists specialize in treating athlete’s foot and offer the best treatment options. If you have any questions about athlete’s foot, consult with Dr. Douglas Mckay from New Jersey . Our doctor will assess your condition and provide you with quality treatment.
What Is Athlete’s Foot?
Tinea pedis, more commonly known as athlete’s foot, is a non-serious and common fungal infection of the foot. Athlete’s foot is contagious and can be contracted by touching someone who has it or infected surfaces. The most common places contaminated by it are public showers, locker rooms, and swimming pools. Once contracted, it grows on feet that are left inside moist, dark, and warm shoes and socks.
Prevention
The most effective ways to prevent athlete’s foot include:
- Thoroughly washing and drying feet
- Avoid going barefoot in locker rooms and public showers
- Using shower shoes in public showers
- Wearing socks that allow the feet to breathe
- Changing socks and shoes frequently if you sweat a lot
Symptoms
Athlete’s foot initially occurs as a rash between the toes. However, if left undiagnosed, it can spread to the sides and bottom of the feet, toenails, and if touched by hand, the hands themselves. Symptoms include:
- Redness
- Burning
- Itching
- Scaly and peeling skin
Diagnosis and Treatment
Diagnosis is quick and easy. Skin samples will be taken and either viewed under a microscope or sent to a lab for testing. Sometimes, a podiatrist can diagnose it based on simply looking at it. Once confirmed, treatment options include oral and topical antifungal medications.
If you have any questions, please feel free to contact one of our offices located in Caldwell, and Galloway, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.